Request a Callback
"*" indicates required fields
United Healthcare
In today’s society, addiction is a widespread issue that affects countless individuals and families. Seeking treatment for addiction can be a challenging journey, both emotionally and financially. That’s why understanding your health insurance coverage is crucial when it comes to addiction treatment.
Whether you or a loved one is struggling with addiction, having a clear understanding of your insurance coverage can make all the difference in getting the help you need. Join Relevance Recovery, as we break down the ins and outs of United Healthcare Insurance’s addiction treatment coverage, empowering you to make informed decisions about your healthcare journey.
Addiction Treatment Coverage
Addiction treatment coverage can vary significantly from one insurance provider to another. When it comes to United Healthcare Insurance, they offer comprehensive coverage for addiction treatment services.
These services include both inpatient and outpatient treatment programs for substance abuse disorders. Inpatient treatment typically involves staying at a specialized facility for a designated period, while outpatient treatment allows individuals to receive care while living at home.
It’s important to note that United Healthcare Insurance covers addiction treatment as part of their mental health and substance abuse benefits. This means that addiction treatment is considered an essential component of overall healthcare coverage, just like any other medical condition.
Types Of Addiction Treatment Covered By United Healthcare Insurance
United Healthcare Insurance recognizes the importance of providing a wide range of treatment options for addiction. The types of addiction treatment covered by United Healthcare Insurance include:
- Detoxification: This is the initial phase of addiction treatment, where the body is rid of harmful substances. United Healthcare Insurance covers medically supervised detoxification programs to ensure the safety and comfort of individuals going through withdrawal.
- Inpatient rehabilitation: United Healthcare Insurance provides coverage for inpatient rehabilitation programs, where individuals receive intensive treatment in a residential setting. These programs often include individual therapy, group therapy, and various evidence-based treatment modalities.
- Outpatient treatment: United Healthcare Insurance also covers outpatient treatment programs. These programs offer flexibility, allowing individuals to receive treatment while still maintaining their daily responsibilities. Outpatient treatment typically includes individual counseling, group therapy, and other supportive services.
- Medication-assisted treatment: United Healthcare Insurance recognizes the effectiveness of medication-assisted treatment for certain substance use disorders. They provide coverage for medications such as methadone, buprenorphine, and naltrexone, which can help individuals manage cravings and withdrawal symptoms.


Coverage Limitations And Restrictions
While United Healthcare Insurance offers comprehensive addiction treatment coverage, it’s important to be aware of any limitations or restrictions that may apply. Some common limitations or restrictions include:
- United Healthcare Insurance may have limitations on the duration of treatment covered.
- It may require individuals to meet specific medical necessity criteria to qualify for coverage.
- In some cases, United Healthcare Insurance may require prior authorization before starting addiction treatment.
In-Network Vs. Out-Of-Network Treatment Providers
In-Network: United Healthcare Insurance has a network of preferred providers, often referred to as in-network providers. These providers have agreed to accept negotiated rates and follow specific guidelines set by the insurance company. It’s generally more cost-effective to receive treatment from in-network providers, as they have established contracts with United Healthcare Insurance.
Out-of-Network: However, United Healthcare Insurance also provides coverage for out-of-network treatment providers. It’s important to note that out-of-network providers may have different reimbursement rates, which could result in higher out-of-pocket costs for policyholders. Before seeking treatment, it’s advisable to check if your preferred providers are in-network or if you need to consider alternatives to minimize your financial responsibilities.
How To Verify Your Insurance Coverage
Before starting addiction treatment, it’s crucial to verify your insurance coverage with United Healthcare Insurance. This will help you understand the specific services covered, any limitations or restrictions, and your financial responsibilities. Here are the steps to verify your insurance coverage:
- Call the customer service number on the back of your insurance card to speak with a representative who can provide detailed information about your coverage.
- Request a summary of benefits document from your insurance provider.
- Review the summary of benefits to understand your co-pays, deductibles, and out-of-pocket expenses.
- Ask your insurance provider for a list of in-network addiction treatment providers.


We believe in Holistic Therapies.
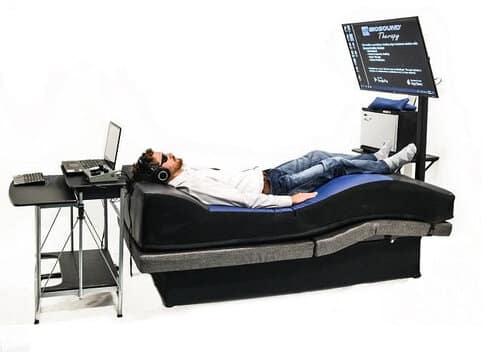
Biosound Therapy
Biosound Therapy is the integration of Biofeedback, Therapeutic Music, sound healing massage, and guided imagery. The guided imagery selections on the Biofeedback Bed are designed to address the guilt, fear, shame and trauma associated as underlying issues for most dealing with addiction. These moving meditations begin with a journey to a completely relaxed state of mind. Then, utilizing a unique echo effect, powerful and positive affirmations are delivered. This combination helps the client overcome those deep rooted, negative patterns of thought and behavior.
- Relieves pain & stress
- Assists with Detoxification Treatment
- Lowers cravings, impulse behavior and racing thoughts
- Lowers anxiety & depression

Equine Psychotherapy
Equine-Assisted Therapy is used to treat patients challenged with everything from drug and alcohol abuse dependency and post-traumatic stress syndrome. The therapy takes advantage of the mental and physical exercise that working with a horse can provide. Equine therapy:
- Helps clients learn to identify and cope with feelings
- Promotes Effective Communication Skills
- Helps Addicts Better Manage Behavior
- Teaches How to Set Boundaries
- Restores Self-Esteem and Self-Worth
*This is an optional, additional therapeutic therapy available after clinical treatment hours.

Massage Therapy
Clients at Relevance receive weekly massage therapy from our Licensed Therapists. Some additional benefits include:
- Release of ‘feel-good’ hormones. According to the American Massage Therapy Association (AMTA), massage helps to increase serotonin and dopamine (feel-good hormones) and decrease cortisol which is related to stress.
- Reduce agitation and anxiety and ease sleep problems.
- Provides a natural, alternative method of healing, free of drugs.
- Helps with the removal of metabolic waste. Therapeutic massage triggers or stimulates the body’s parasympathetic nervous system. This in turn can increase circulation and promote the effectiveness of the lymph system. The lymph system helps to alleviate pain symptoms and is responsible for removing the body’s metabolic waste build-up.
- Provides the client with a connection to their body, and improves or increases body awareness.
Navigating The Pre-Authorization Process
For certain addiction treatment services, United Healthcare Insurance may require pre-authorization before treatment can begin. Here’s how to navigate the pre-authorization process
- Work closely with your healthcare provider to gather all the necessary documentation to support the need for addiction treatment.
- Your healthcare provider will submit the pre-authorization request to United Healthcare Insurance on your behalf.
- After submitting the pre-authorization request, follow up with your insurance provider to ensure that it is being processed.
- Once the pre-authorization request is approved, you will receive confirmation from your insurance provider.


Co-Pays, Deductibles, And Out-Of-Pocket Expenses
When it comes to addiction treatment, it’s essential to understand your co-pays, deductibles, and out-of-pocket expenses. Here’s a breakdown of these terms:
- Co-pays: A co-pay is a fixed amount that you are required to pay for certain services, such as a doctor’s visit or a therapy session. The co-pay amount may vary depending on the specific service and your insurance plan.
- Deductibles: A deductible is the amount you must pay out-of-pocket before your insurance coverage kicks in. For example, if you have a $1,000 deductible, you will be responsible for paying the first $1,000 of your addiction treatment costs before your insurance starts covering a portion of the expenses. It’s important to note that deductibles can vary based on your insurance plan.
- Out-of-pocket expenses: Out-of-pocket expenses refer to the costs that you are responsible for paying directly, beyond any co-pays or deductibles. These expenses can include co-insurance, which is a percentage of the total cost that you are required to pay, as well as any costs that exceed your policy’s coverage limits.
Finding Treatment Providers That Accept United Healthcare Insurance
To ensure that you receive the maximum benefits from your United Healthcare Insurance coverage, it’s important to find addiction treatment providers that accept your insurance. Here are some steps to help you find providers:
- United Healthcare Insurance provides an online directory of in-network providers.
- If you’re having trouble finding suitable providers or need assistance, don’t hesitate to reach out to your insurance provider. They can provide you with additional recommendations.
- Reach out to your healthcare provider, therapist, or support groups for recommendations that accept United Healthcare Insurance.
- Once you’ve identified potential addiction treatment providers, verify their credentials. Check if they are licensed, accredited, and experienced in treating substance abuse disorders.
Next Steps Towards Recovery
Remember to verify your insurance coverage, understand your financial responsibilities, and find addiction treatment providers that accept United Healthcare Insurance. By taking these steps, you can focus on your recovery without the added stress of financial burdens.
Don’t hesitate to reach Relevance Recovery for help, if you or someone you know is struggling with addiction.
Get the Help You Need, Now.
Start your journey to substance abuse recovery with us in New Jersey today.





