In the intricate landscape of mental health, Borderline Personality Disorder (BPD) stands as a unique and often misunderstood entity. This enigmatic condition weaves a complex tapestry of emotions, behaviors, and thoughts that can be both bewildering and challenging for those who experience it and those who seek to understand it.
It is a complex mental health condition that impacts how an individual views themselves and others in their lives. It is characterized by – intense mood swings, impulsive behavior, extreme anger, unstable relationships, and a distorted self-image. BPD might feel as if everything about an individual is unstable. People with BPD say that having BPD feels like having an exposed nerve ending, which makes them highly sensitive and triggered by the smallest of things. These triggers can trigger intense emotional reactions, leading to impulsive actions and strained interpersonal connections.

Recognizing Symptoms
Recognizing the symptoms of BPD is pivotal, as it enables a better understanding of the challenges faced by individuals dealing with this disorder and encourages a supportive environment. Early intervention and treatment is crucial for any individual.
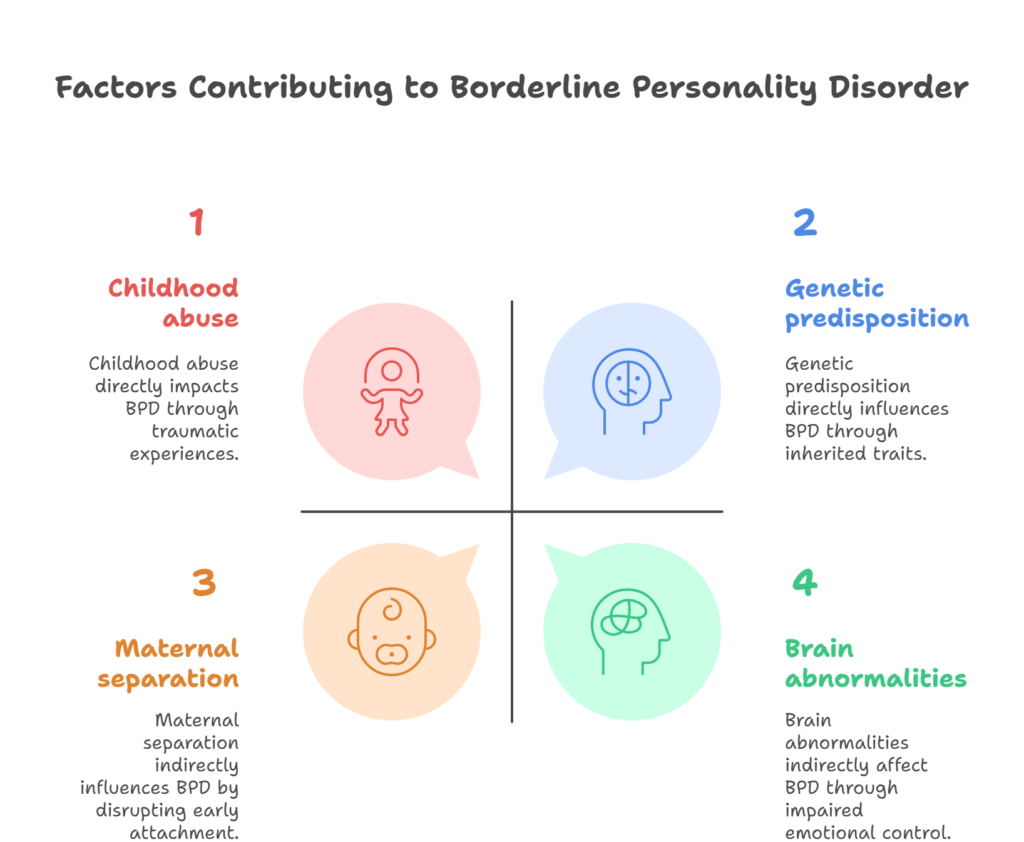
BPD may be caused by environmental factors like child abuse or neglect, inherited genetic conditions, or brain abnormalities. By raising awareness about the symptoms of BPD, we can contribute to a more empathetic and inclusive environment for individuals navigating the complexities of this disorder. In this blog, we embark on a journey to decode the mysteries of BPD by exploring its symptoms, shedding light on its intricacies, and offering insights into how to navigate this challenging terrain with empathy and understanding.
Symptoms of BPD
Timely symptom recognition can help individuals maintain a higher quality of life. Effective management of symptoms can alleviate discomfort and enhance overall well-being. Identifying symptoms promptly allows for early medical intervention. This can prevent a condition from worsening and increase the chances of successful treatment. We can measure the symptoms of BPD on the following scales and closely observe how this condition has different impacts in different situations.
1. Relationship Instability
If someone you know has intense, short-term, unstable relationships, they might be suffering from BPD. People with BPD also tend to be misunderstood by others due to their actions driven by intense anger, fear of abandonment, and lack of self-image. These emotional fluctuations can lead to misunderstandings and conflicts, making it difficult for them to form stable relationships.
2. Extreme Emotional Volatility
Little things in life that might not matter to others can bring extreme emotions in individuals with BPD. These emotions are not different from others, just more intense, fluctuating, and unpredictable than others. These feelings could be so intense that BPD patients try to numb them using other self-destructive behaviors.
These emotions may last for a couple of days or they may leave instantly. They also struggle with emotional regulation, making it difficult for them to manage their moods effectively. Their mood can shift at any moment, so quickly that sometimes one cannot even understand what the trigger was. All this can confuse the people around and may have a serious impact on the life of the individual and the relationship with their family and friends.
3. Self-harm
People with BPD engage in thoughts of suicide and also make suicidal gestures and threats. They tend to engage in other behaviors that deliberately harm themselves unrelated to suicide, like dangerous and unhealthy binge drinking or binge eating, cutting themselves or causing other self-injuries, using drugs, often engaging in unsafe sex, etc.
They do so to feel better at the moment, to feel in control of their pain, to punish themselves or someone else, or to show how they are actually feeling inside. Self-harm provides temporary relief but it leads to even more shame and self-hatred. National Alliance on Mental Illness says that ~75% of BPD patients will attempt self-harm at some point, underlining the severity of this symptom.
4. Disconnected with Reality and Feelings of Emptiness
Individuals diagnosed with BPD often feel suspicious or paranoid about other people’s intentions. When stressed, they feel dissociated from reality, which looks like being spaced out, foggy, or as if the person exists outside their body.
While other intense emotions may come and go, one feeling stays; feelings of emptiness. There is no genuine sense of self which leads to feeling even more lonely and isolated.
5. Intense fear of Abandonment and Rejection
This is the hallmark trait of borderline personality disorder, and it is common for BPD patients to have post-traumatic stress disorder related to abandonment. It is this fear that drives other behaviors. What others might feel as normal, BPD patients may not, and that could lead to misunderstandings and rifts, making them feel even more alone.
These fears can come out as clinginess, possessiveness, anger, or an attempt to cancel other people’s plans as a way to cope with the perceived threat of abandonment. But one can always learn to understand and navigate their emotions, strengthening their relationship instead of damaging it.
What causes borderline personality disorder?
Common BPD Triggers and Identifying an Episode
Some common triggers for borderline personality disorder diagnosed individuals are perceived or real abandonment or rejection, reminders of traumatic events, locations invoking negative memories, etc. Certain locations, objects, or even specific smells can evoke distressing memories, reopening emotional wounds and causing significant distress. These triggers transport individuals back to the painful moments of their past, amplifying feelings of helplessness and despair. They can lead to emotions of self-loathing or low-self image, which can further trigger anger or actions of self-harm.
BPD episodes are different for different individuals but there are certain common themes like intense outbursts of anger, depression, anxiety, withdrawal, or avoidance. 80% of those suffering from BPD experience suicidal thoughts and behavior while in the throes of an episode as well. They also get thoughts of everyone hating them and being against them. But they don’t experience the extremes of negative emotions only. BPD episodes can also look like extreme euphoria or positive emotions. Hence, reaching out to a licensed mental health professional in time is critical.
FAQs
1. What are some misconceptions and myths related to borderline personality disorder?
Some people believe that BPD is not treatable; borderline personality disorder diagnoses are always child abuse victims, and it happens more often in women than men. None of these myths are true.
In recent times, many treatments and therapies have proven to manage and even treat BPD successfully. While a history of trauma can contribute to the development of BPD, it’s not the sole cause. Borderline personality disorder can occur due to other factors like genetics or brain abnormalities, and it is equally likely to occur in both men and women.
2. What are the common treatments for BPD?
There are typically four types of therapies involved in treating BPD – GPM, DBT, MBT, and TFP. General Psychiatric Management (GPM) is designed to provide “good enough” treatment to BPD patients and is enough in most cases. Dialectical Behavioral Therapy (DBT) helps develop four skill sets: mindfulness, interpersonal effectiveness, emotion regulation, and distress tolerance. DBT equips individuals with practical tools to manage intense emotions and improve their relationships.
Mentalization-based treatment (MBT) helps improve interpersonal relationships by focusing on the emotional state of mind. By developing a deeper understanding of emotions and their impact on relationships, individuals with BPD can foster healthier connections with others. Transference-focused Psychotherapy (TFP) focuses on restoring the individual’s sense of self by helping them verbalize their emotions, leading to a more stable self-identity.
3. How do I manage BPD triggers?
Apart from seeking treatment, here are a few ways to manage BPD triggers – take a warm shower, play relaxing music, engage in physical activities, express yourself using creative means like drawing, painting, or writing, try relaxation exercises, or attend therapy sessions.
Conclusion
It can be extremely challenging to be someone and to be with someone with borderline personality disorder. However, with proper medical support and treatment, one can learn to communicate feelings and overcome negative symptoms. It will help in building and maintaining a happy and fulfilling relationship with self and with others. Having a team of experts behind you who can help you get out of this rabbit hole is a blessing.
We, at Relevance Recovery are constantly working hard to provide the best medical support and treatment to patients with borderline personality disorder via our borderline personality outpatient program. This is a program that allows you to engage in therapy while going about the tasks of everyday life. You can even opt-in for partial hospitalization which requires you to stay in the facility from 9 AM to 3 PM. During this time, you are made to follow a therapy program that is customized to your specific needs. It aims to target the source of your disorder and find healthy coping mechanisms to replace unhealthy behavior.
In worst-case scenarios, patients may also go through an assisted detox to rid their bodies of harmful toxins before they start therapy.
Sources
- BPD Treatment Triggers
- Recognizing the Signs of BPD
- BPD Essentials